What is CRVO?
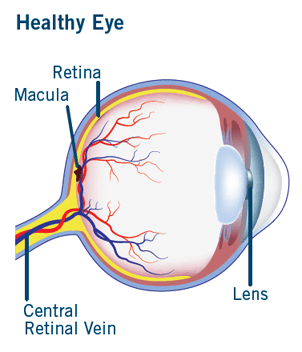
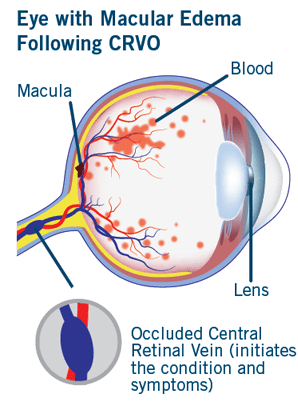
Veins return oxygen-depleted blood back to the heart. The retina has one major artery and one major vein. The vein is called the central retinal vein. Central retinal vein occlusion (CRVO) is a blockage of this vein that causes the vein to leak blood and excess fluid into the retina. This fluid often collects in the area of the retina responsible for central vision called the macula. When the macula is affected, central vision may become blurry.
Who is at Risk for CRVO?
After diabetic retinopathy, CRVO is the second most common retinal vascular disorder. CRVO usually occurs in people who are aged 50 and older. In most cases, it is not known what causes the condition. It is more common in patients with high blood pressure, arteriosclerosis, diabetes, and glaucoma than it is in other people.The second eye will develop vein occlusion in 6-17% of cases.
What are the signs and symptoms of CRVO?
CRVO causes sudden, painless vision loss in one eye that can become worse over several hours or days.
What are the types of CRVO?
There are two types of CRVO:
- Non-ischemic CRVO is a less serious form of CRVO, which accounts for about 75% of cases, and usually has a better visual outcome.
- Ischemic CRVO is a more serious form of CRVO that can lead to the development of significant complication, vision loss and possibly loss of the eye.
How Does CRVO Damage My Eyes?
Fluid collects in the area of the retina responsible for central vision called the macula. The fluid causes swelling or edema of the macula, causing a person’s central vision to become blurry. This condition is called macular edema. Some of the most common signs of macular edema following CRVO are blurred vision, distorted vision, or vision loss in all or part of the eye.
The retina can become starved for oxygen (ischemia), leading to growth of abnormal blood vessels. Some people with ischemic CRVO develop neovascular glaucoma, where abnormal blood vessels cause an increase in eye pressure that can cause pain and severe vision loss. It can take three months or longer for neovascular glaucoma to occur after the development of CRVO.
How Do Eye Doctors Check for CRVO?
If you have sudden vision loss, contact an eye care professional immediately. At the exam, the eye doctor will widen (dilate) the pupil of the eye with eye drops to allow a closer look at the inside of the eye and the retina to determine if you have CRVO.
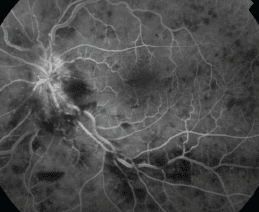
An eye doctor can also determine potential damage caused by CRVO by performing a test called fluorescein angiography. During this test, a dye is injected into the arm that “lights up” the blood vessels in the eye while multiple photos are taken of the back of the eye. This type of photography provides a clear picture of the retinal blood vessels for diagnosis. Additional tests may include imaging to determine the extent of swelling in the macula.
Fluorescein Angiography
The eye doctor may also test vision, the light reflex of your eye, eye pressure, and your side (peripheral) vision. An examination of the internal structures of your eye may be performed and additional photos may be taken.
The doctor will recommend a thorough medical examination to determine if other conditions exist by checking your blood sugar, cholesterol levels, blood pressure, and possibility of cardiovascular disease.
CRVO Treatment
Most patients with CRVO, especially the ischemic type, have some reduced central vision, although some may regain some vision without treatment. It is important to determine the cause of the blockage through a medical evaluation. There is no treatment available for CRVO but there are treatments for the complications related to CRVO.
Injectable medications and steroids can be used to treat macular edema. Laser treatment called panretinal photocoagulationis used to prevent neovascular glaucoma. This procedure uses a laser beam to treat many places on the retina. This technique helps prevent the growth of new, abnormal blood vessels.
Those with CRVO need to see an eye doctor at regular intervals to monitor for neovascular glaucoma and should be seen earlier and more frequently if there is a noticeable decrease in vision or eye pain.
Prevent Blindness and Your Eyes
Prevent Blindness is the patient advocate for healthy vision. We educate people about their risk of eye disease and steps they can take to protect their sight. We promote access to eye care and support research into the prevalence, cost, and cure of eye disease. Find out more about us, and please consider a tax-deductible donation to give the gift of sight and help more Americans enjoy healthy vision for life.