What is diabetic retinopathy?
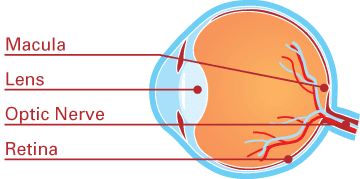
Diabetes-related retinopathy (or diabetic retinopathy) occurs when small blood vessels leak and bleed in the retina. The retina is layer of the eye that acts like the film in the camera of the eye to help you see. Diabetes-related retinopathy is a leading cause of blindness in American adults and it affects over one in four of those living with diabetes, while 4% have severe cases of retinopathy.


Download Diabetic Retinopathy Fact Sheets:
Diabetes & Your Eyes – Diabetic Retinopathy – Symptoms + Risks
Diabetes & Your Eyes – Diabetic Retinopathy – Diagnosis, Treatment, & Prevention
What are the Symptoms of Diabetic Retinopathy?
Early detection and treatment can reduce your risk of diabetes-related retinopathy. You will usually not experience symptoms in the early stages, which is why it is important for you to have an eye exam annually, or as directed by your doctor. Eye exams can be done either through a dilated eye exam with an eye doctor (preferred method) or through photos of the retina in each eye, which may not require dilation of the eyes.
Vision changes due to diabetes-related eye disease usually affects both eyes. Here are some symptoms you can look for:
Diabetes Resources at Prevent Blindness
These resources are designed to support individuals living with diabetes and help them gain access to eye care that they require to maintain healthy vision.
Vision changes due to diabetes-related eye disease usually affects both eyes. Here are some symptoms you can look for:
Sudden increase in eye floaters (spots and/or dark cobweb-like strands)
Blurred vision
Sudden loss of vision in one eye
Halos around lights
Flashing lights
Poor night and color vision
What Decreases and Increases Your Risk for Diabetes-related Retinopathy?
If you have diabetes, there are different factors that can decrease and increase your risk for developing diabetes-related retinopathy. Your risk depends on:
Duration of the Disease
The longer you have diabetes, the greater your risk for developing diabetes-related retinopathy.
Blood glucose management
Blood glucose management will decrease your risk for diabetes-related retinopathy and vision loss. Work with your healthcare provider to be sure your glucose level is in your recommended target range.
Race
Some racial and ethnic groups are at higher risk. If you are African American, Hispanic, American Indian, Asian American, or Pacific Islander, you are at increased risk for developing diabetes-related retinopathy.
Smoking
Smoking increases your risk. If you don’t smoke, be sure you do not start. If you do smoke, ask your doctor how to help you quit.
Blood pressure and cholesterol

By managing your blood pressure and cholesterol you will decrease your risk of eye disease. You will also protect your heart, kidneys, feet, ears, and eyes. Eat a healthy diet, get regular exercise and/or take medication as prescribed by your doctor to manage your blood pressure and cholesterol levels. These steps will help you reduce your risk of diabetes-related retinopathy.
Pregnancy
If you have diabetes prior to getting pregnant, see your eye doctor regularly to prevent risks of developing diabetes-related retinopathy. If you develop gestational diabetes during pregnancy, your risks are much lower and you are not required to get an eye examination.
Kidney Disease
There is a close relationship between kidney disease and diabetes-related retinopathy. Preventing complication with your kidneys will also help prevent diabetes-related retinopathy.
How is Diabetes-related Retinopathy Diagnosed?
If you have diabetes, you should have an eye exam which includes dilation at least once a year, or more often as recommended by your eye doctor (an ophthalmologist or optometrist). Your eye examination should include dilation. Dilation of the eyes is done using eye drops to widen the opening on the front of your eye, called the pupil. This allows the eye doctor to see into the back of the eye. This is an important step to take when getting an eye exam for people living with diabetes. The temporary side effects of dilation eye drops are blurring of vision, especially up close, and sensitivity to light. The effects only last a few hours or less, but the benefit can be enormous!
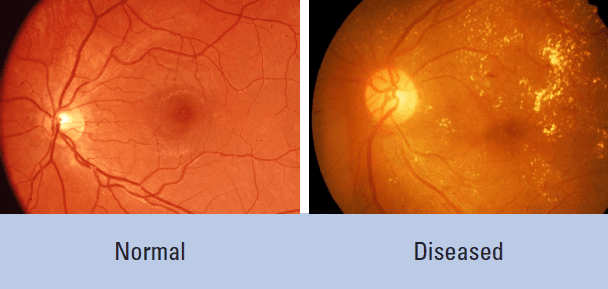
The photo at right shows a retina damaged by diabetes-related retinopathy
If for some reason you cannot fit in an annual dilated eye exam, work with your primary care doctor to have photos taken of your retina in each eye to screen for diabetes-related eye disease. These photos are examined by an eye doctor to determine if you might have diabetes-related eye disease. Your photos can be used to compare to images taken in past and future exams. This helps monitor the health of your eye to determine if you have retinopathy and need a complete dilated eye exam. Your eye doctor can then use the pictures to show you what is happening in your eye so, together, you can develop a treatment plan. Timely treatment of diabetesrelated retinopathy can help reduce your risk for vision loss.
How is Diabetes-related Retinopathy Treated?
In the early stages of diabetes-related retinopathy, annual dilated eye exams (or more often as recommended by the eye doctor) are important for monitoring retinopathy.
In more advanced stages, you have a range of options for treatment, including:
- medications
- laser procedures
- surgery
Talking with your eye doctor and working together on your treatment plan is the best way to determine the next steps that are right for you.
It is important that you know that damage in your retina often happens before you notice changes in your vision. Having a dilated eye exam annually (or at least retinal photographs evaluated by an eye doctor) is the best way to catch any eye disease in its early stage to ensure you have healthy vision. Your eye doctor will talk with you if you need an eye exam more than once a year and/or to discuss any treatment you may need.
How Can You Keep Your Eyes Healthy When You Have Diabetes?
Know your numbers to manage your glucose, blood pressure, and cholesterol levels.
Get a dilated eye exam annually, or more often as recommended by the eye doctor. If you cannot get an eye exam annually, work with your primary health doctor to obtain photos of your retina in each eye. These photos are examined by an eye doctor to determine if you might have diabetes-related eye disease.
Maintain a healthy lifestyle. This should include regular exercise, not smoking, and following a healthy meal plan. Talk to a dietitian or diabetes educator about your eating habits and creating an exercise routine. There are a lot of wonderful recipes and fitness resources to help you!
Additional Fact Sheets in English and Spanish
Right-click the links to download the files.
English
Diabetes & Your Eyes – Diabetes-related Retinopathy – Symptoms + Risks (English)
Diabetes & Your Eyes – Diabetes-related Retinopathy – Diagnosis, Treatment, & Prevention (English)
Spanish
La Diabetes y Sus Ojos – Retinopatía relacionada con la diabetes – Síntomas y riesgo (en español)
Diabetes & the Eyes Educational Toolkit
The Diabetes & the Eyes Educational Toolkit offers educational materials on diabetes and the impact of diabetes on eye health in both English and Spanish. These educational resources are intended for healthcare professionals, community health educators, diabetes educators, and anyone in a caregiving or diabetes education role. The English version of the educator course and the factsheets have received Favorably Reviewed Approval from the American Association of Diabetes Educators (AADE).
Living Well with Low Vision is an online resource to educate those with loss of vision on how maintain their independence and quality of life.